White Gums: Understanding the Causes, Implications, and Treatment Options
The presence of white gums, medically termed leukoplakia (when the white patch is not easily scraped off) or simply white patches on the gums (when easily scraped off), can signal a range of oral health issues, from relatively benign conditions to more serious underlying diseases. Understanding the potential causes, recognizing the symptoms, and seeking appropriate medical attention are crucial steps in ensuring proper diagnosis and effective treatment. This article provides a comprehensive overview of white gums, outlining potential causes, associated risks, diagnostic procedures, and available treatment options.
Potential Causes of White Gums
The appearance of white patches or discoloration on the gums can stem from various factors, ranging from simple irritations to more serious underlying medical conditions. Accurate diagnosis is paramount, as treatment strategies vary significantly depending on the underlying cause.
Oral Hygiene and Irritants
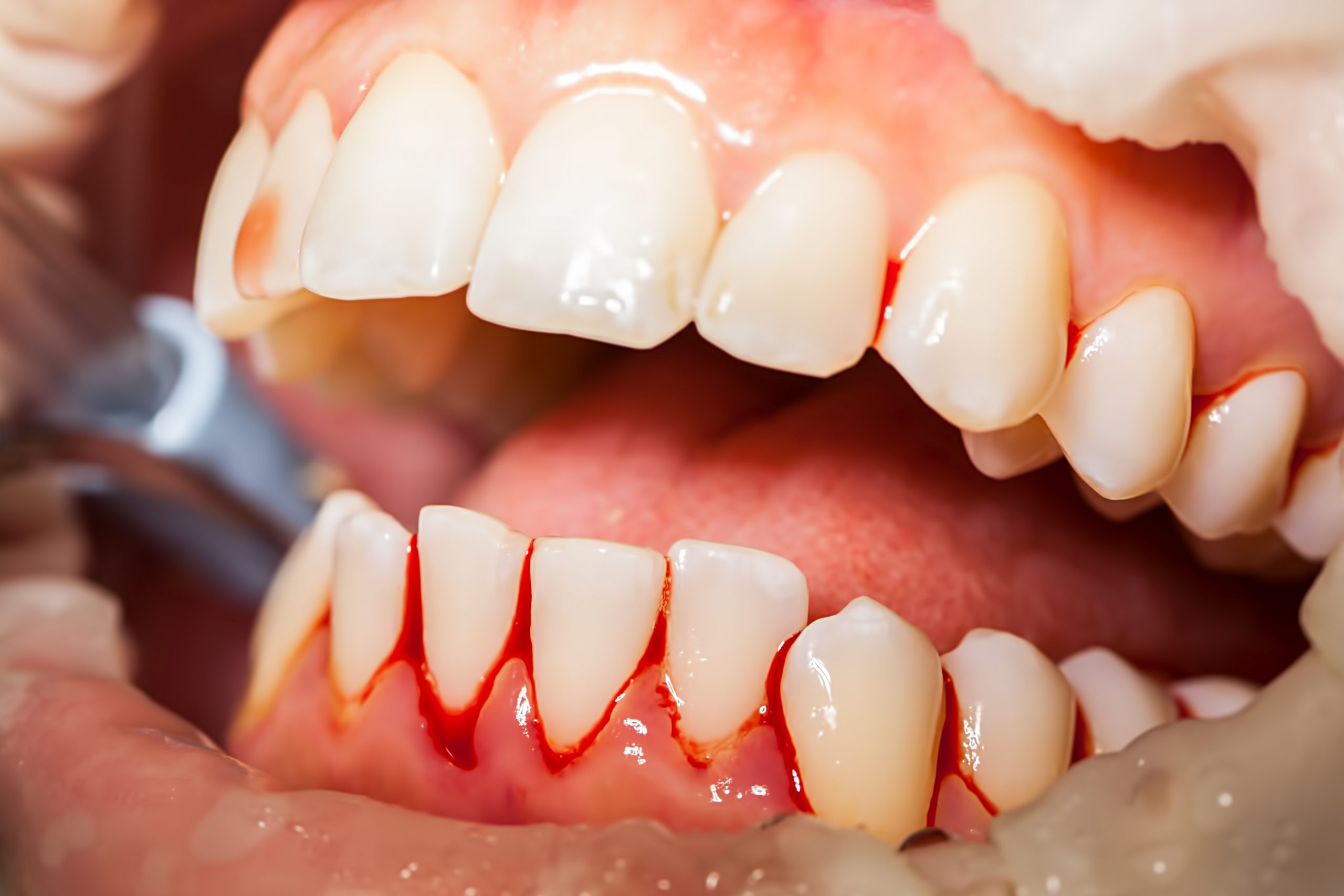
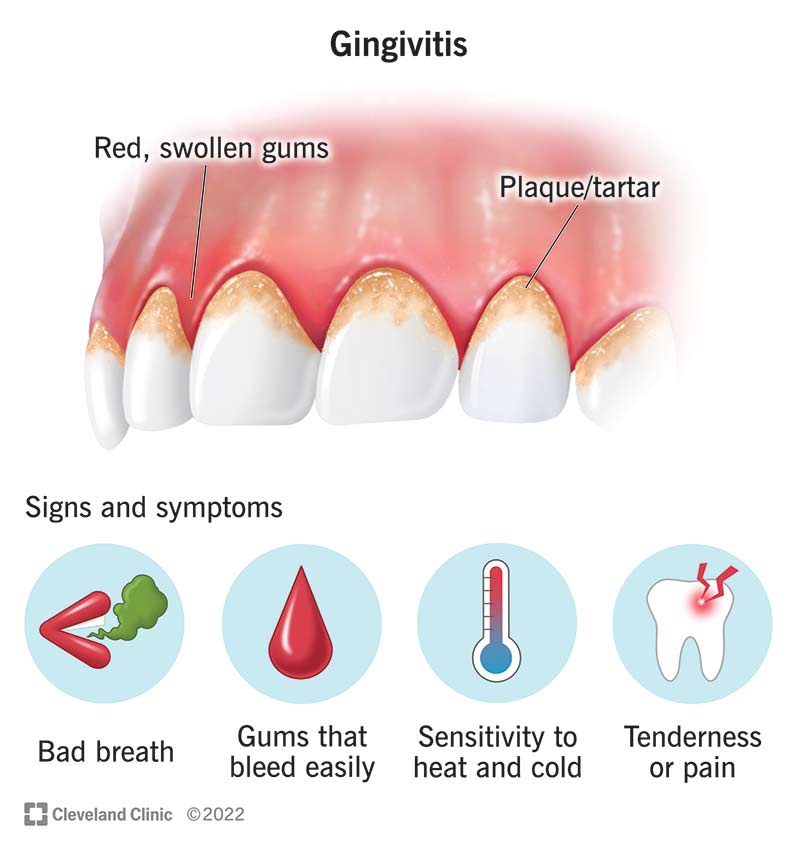
Poor oral hygiene is a common culprit. The accumulation of plaque and tartar can irritate the gum tissues, leading to inflammation (gingivitis) and potentially causing white patches. These patches are often accompanied by redness, swelling, and bleeding gums. Similarly, the use of harsh mouthwashes, abrasive toothpastes, or ill-fitting dentures can cause irritation and lead to the development of white patches. Improper brushing techniques, excessive scrubbing, and the use of hard-bristled toothbrushes can also contribute to this problem.
Fungal Infections
Oral candidiasis, commonly known as thrush, is a fungal infection caused by an overgrowth of Candida albicans, a yeast normally present in the mouth. While thrush can manifest in various ways, including creamy white patches, it frequently affects the gums, causing them to appear white and often exhibiting a cottage cheese-like texture. Individuals with weakened immune systems, such as those with HIV/AIDS, diabetes, or undergoing chemotherapy, are at a higher risk of developing oral candidiasis.
Lichen Planus
Lichen planus is a chronic inflammatory condition that can affect the skin and mucous membranes, including the gums. It presents as lacy white patches or streaks on the gums, sometimes accompanied by ulcerations and burning sensations. The exact cause of lichen planus remains unknown, but it's believed to involve an autoimmune response.
Leukoplakia
Leukoplakia is characterized by white patches or plaques on the mucous membranes that cannot be easily scraped off. While some forms of leukoplakia are benign, others can be precancerous and potentially progress to oral cancer. Risk factors for leukoplakia include tobacco use, excessive alcohol consumption, and chronic irritation from ill-fitting dentures. Regular dental checkups and prompt attention to any persistent white patches are crucial for early detection and intervention.
Oral Cancer
In more serious cases, white patches on the gums can be an early sign of oral cancer. While not all white patches indicate cancer, persistent, unexplained white lesions warrant immediate medical attention. Risk factors for oral cancer include tobacco use (smoking and chewing tobacco), excessive alcohol consumption, exposure to the human papillomavirus (HPV), and a family history of oral cancer. Early detection through regular dental examinations and prompt treatment are vital in improving prognosis.
Diagnostic Procedures
Diagnosing the underlying cause of white gums requires a thorough clinical examination by a dentist or oral surgeon. The following procedures may be employed:
- Visual Inspection: The dentist will visually examine the gums, noting the appearance, texture, and location of the white patches.
- Medical History Review: A comprehensive medical history, including information on medications, lifestyle habits (tobacco and alcohol use), and overall health, will be obtained.
- Scraping Test: The dentist may attempt to scrape off the white patch. If it's easily removed, it's less likely to be a serious condition. If it's firmly attached, further investigation may be necessary.
- Biopsy: In cases where the cause remains unclear or if there's a suspicion of leukoplakia or oral cancer, a biopsy may be performed. A small tissue sample is taken and sent to a laboratory for microscopic examination.
- Blood Tests: Blood tests may be ordered to assess overall health and rule out underlying medical conditions.
Treatment Options
Treatment for white gums depends entirely on the underlying cause. Effective management necessitates accurate diagnosis.
Addressing Oral Hygiene Issues
For white patches resulting from poor oral hygiene, improved brushing and flossing techniques, along with the use of a fluoride toothpaste, are often sufficient to resolve the issue. The dentist might also recommend a therapeutic mouthwash to help reduce inflammation and bacterial load.
Treating Fungal Infections
Oral thrush is typically treated with antifungal medications, either in the form of topical creams or oral tablets. The duration of treatment depends on the severity of the infection.
Managing Lichen Planus
Lichen planus treatment focuses on managing symptoms and preventing complications. This may involve topical corticosteroids, antihistamines, or other medications to reduce inflammation and alleviate discomfort. Regular monitoring is essential.
Treating Leukoplakia
Treatment for leukoplakia depends on whether it's benign or precancerous. Benign leukoplakia may require no specific treatment beyond regular monitoring. Precancerous leukoplakia may require surgical removal of the affected tissue or other interventions such as laser therapy.
Oral Cancer Treatment
Treatment for oral cancer depends on the stage and extent of the cancer. Options may include surgery, radiation therapy, chemotherapy, or a combination of these modalities. Early detection significantly improves the chances of successful treatment and recovery.
Preventive Measures
Maintaining good oral hygiene is crucial in preventing many causes of white gums. This includes:
- Brushing teeth twice daily with fluoride toothpaste.
- Flossing daily to remove plaque and food particles between teeth.
- Using a soft-bristled toothbrush and gentle brushing techniques.
- Regular dental checkups and professional cleanings.
- Limiting alcohol consumption and avoiding tobacco use.
- Maintaining a healthy immune system.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. If you experience white gums or any other oral health concerns, consult a dentist or other qualified healthcare professional for proper diagnosis and treatment. Early detection and intervention are crucial for managing oral health issues effectively.