
The Synergistic Role of Probiotics in Enhancing Oral Health
Maintaining optimal oral hygiene is paramount for overall health and well-being. While traditional methods like brushing and flossing remain essential, emerging research highlights the significant contribution of probiotics to strengthening teeth and promoting gum health. This article explores the multifaceted mechanisms by which probiotics exert their beneficial effects on the oral microbiome, contributing to a healthier and more resilient oral cavity over time.
Understanding the Oral Microbiome and its Dysbiosis
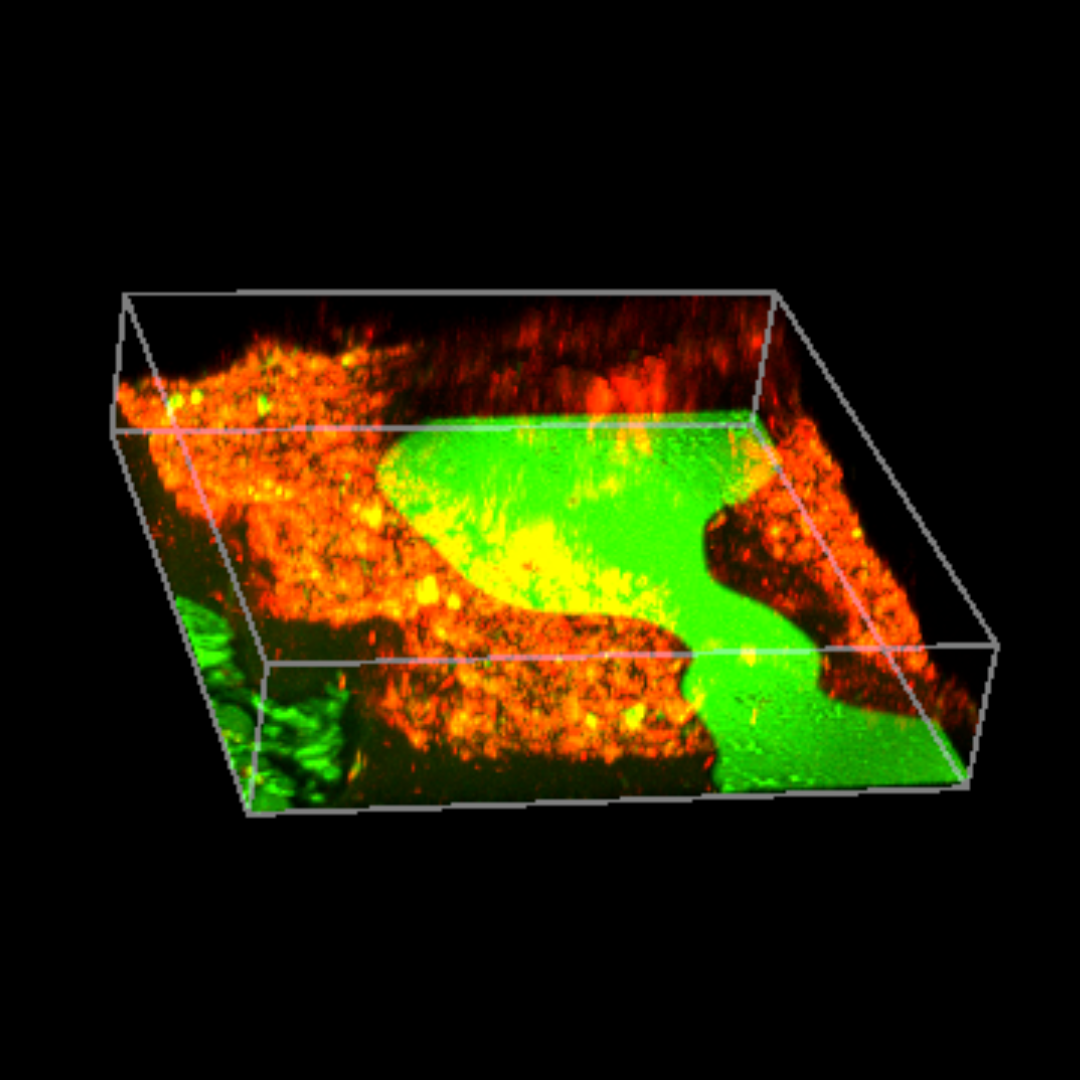
The human mouth harbors a complex and dynamic ecosystem of microorganisms, collectively known as the oral microbiome. This intricate community comprises bacteria, archaea, fungi, viruses, and protozoa, each playing a specific role in maintaining oral health. A balanced oral microbiome, characterized by a diverse array of beneficial species, contributes to the effective prevention of pathogens and the maintenance of gingival integrity. However, disruptions in this delicate balance, termed dysbiosis, can lead to the proliferation of harmful bacteria and the development of various oral diseases.
The Role of Dysbiosis in Periodontal Disease
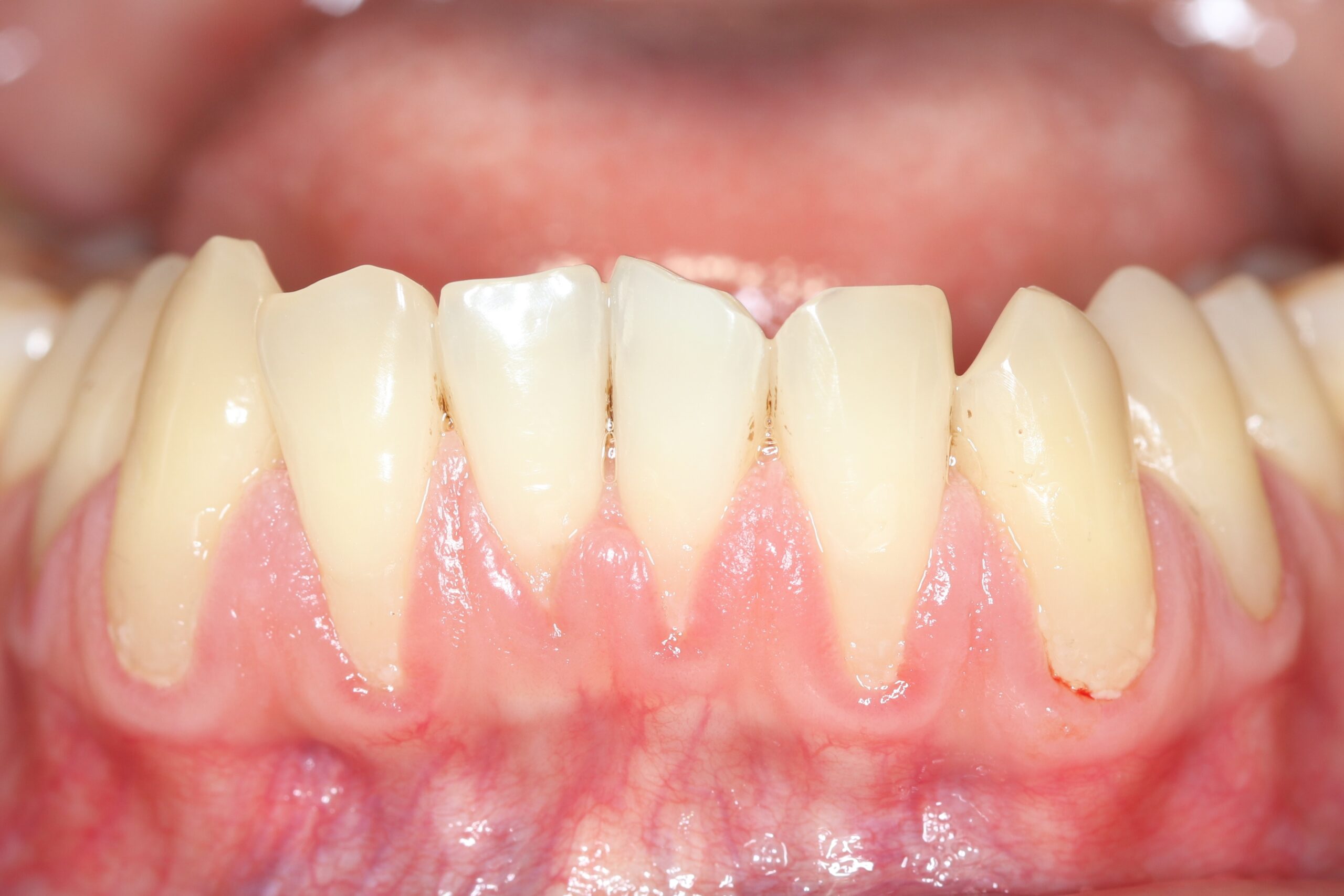
Periodontal disease, encompassing gingivitis and periodontitis, is a prevalent inflammatory condition affecting the supporting structures of the teeth. Dysbiosis plays a central role in the pathogenesis of periodontal disease. An imbalance favoring pathogenic bacteria, such as Porphyromonas gingivalis, Aggregatibacter actinomycetemcomitans, and Tannerella forsythia, leads to chronic inflammation, alveolar bone loss, and ultimately, tooth loss. These bacteria produce various virulence factors, including enzymes that degrade collagen and other connective tissues, contributing to the destruction of periodontal tissues.
The Impact of Dysbiosis on Caries Formation
Similarly, dental caries, or tooth decay, is significantly influenced by the composition of the oral microbiome. The acidogenic bacteria, primarily Streptococcus mutans and Lactobacillus species, metabolize dietary carbohydrates, producing organic acids that demineralize tooth enamel, leading to the formation of caries lesions. Dysbiosis, marked by an overgrowth of these acidogenic and acid-tolerant bacteria, predisposes individuals to increased caries susceptibility.
Probiotics: Restoring Balance to the Oral Microbiome
Probiotics, defined as live microorganisms that confer a health benefit on the host when administered in adequate amounts, offer a promising approach to modulating the oral microbiome and preventing or treating oral diseases. Several mechanisms underpin the beneficial effects of probiotics on oral health:
Competitive Exclusion and Inhibition of Pathogens
Probiotics exert their beneficial effects, in part, through competitive exclusion. By occupying available binding sites on the tooth surface and epithelial cells, probiotics prevent the colonization and proliferation of pathogenic bacteria. Furthermore, certain probiotic strains produce antimicrobial substances, such as bacteriocins, hydrogen peroxide, and organic acids, that directly inhibit the growth and activity of harmful bacteria. This competitive antagonism contributes to a reduction in the overall pathogenic burden within the oral cavity.
Modulation of the Immune Response
Probiotics interact with the host immune system, influencing the inflammatory response and promoting tissue repair. They can stimulate the production of antimicrobial peptides and cytokines, enhancing the host's defense against pathogenic bacteria. Furthermore, some probiotic strains have been shown to reduce the levels of inflammatory mediators, such as prostaglandins and interleukins, thereby mitigating the inflammatory response associated with periodontal disease.
Enhancement of Salivary Factors
Saliva plays a crucial role in maintaining oral health through its buffering capacity, antimicrobial properties, and remineralization potential. Certain probiotic strains have been shown to positively influence salivary parameters. They may increase salivary flow rate, enhance the concentration of antimicrobial compounds such as lysozyme and lactoferrin, and improve the buffering capacity of saliva, thereby contributing to a more protective oral environment.
Specific Probiotic Strains and Their Oral Health Benefits
Several probiotic strains have demonstrated promising results in preclinical and clinical studies regarding their impact on oral health. These include, but are not limited to:
- Lactobacillus reuteri: Studies suggest its effectiveness in reducing Streptococcus mutans levels and improving salivary parameters.
- Lactobacillus rhamnosus: Demonstrates potential in reducing gingival inflammation and improving periodontal parameters.
- Streptococcus salivarius K12: Known for its ability to inhibit the growth of pathogenic bacteria such as Streptococcus mutans and Aggregatibacter actinomycetemcomitans.
- Weissella cibaria: Exhibits potential in reducing plaque accumulation and gingival inflammation.
It is important to note that the efficacy of different probiotic strains can vary, and further research is necessary to determine the optimal strains and dosages for various oral health conditions.
Delivery Methods and Future Directions
Probiotics can be administered through various methods, including oral supplements (capsules, tablets, powders), chewing gums, lozenges, and mouthwashes. The choice of delivery method depends on factors such as patient preference, the specific probiotic strain, and the targeted condition. Future research should focus on optimizing delivery systems to ensure the viability and efficacy of probiotic strains within the oral cavity.
Furthermore, personalized approaches to probiotic therapy are needed to consider individual variations in the oral microbiome and host response. Advanced techniques, such as next-generation sequencing and metagenomics, can be utilized to characterize the oral microbiome and identify specific probiotic strains tailored to individual needs. This personalized approach promises to maximize the efficacy of probiotic interventions and enhance their contribution to overall oral health.
In conclusion, accumulating evidence supports the beneficial role of probiotics in promoting gum health and strengthening teeth over time. By modulating the oral microbiome, enhancing the host immune response, and improving salivary factors, probiotics contribute to a more resilient and balanced oral ecosystem. While further research is needed to optimize the use of probiotics for various oral health conditions, their incorporation into comprehensive oral hygiene regimens holds significant promise for improving oral health outcomes and preventing oral diseases.



.jpg)







